
Denial Defects and Denial Management
Remittance denials greatly impact the revenue cycle by delaying or reducing payments from payors to providers. While denials can cause a significant amount of revenue loss, most of them can be avoided.
Denials are simply the result of a rules-set, programmed within the payor system to look for matching information in a myriad of patient and contract databases. ReMedics improves the claim process by helping to stop recurring denials — with reporting & analytics tools to help identify the root cause of problem areas.
While ReMedics goal is to prevent denials from occurring altogether, we provide our clients with the right workflow efficiency tools to quickly get them appealed and resolved.
Denial Analysis Scorecards
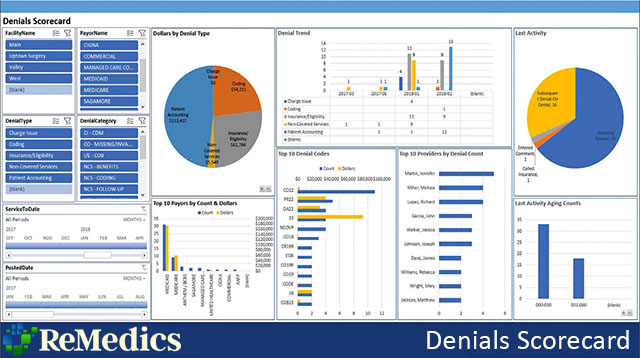
Denials trends can be analyzed and traced to specific areas, from patient access and eligibility to individual physicians, departments or type of service.
By providing a complete record of all denials, with Power BI drill-down capabilities, we provide valuable insight into where errors are more likely to occur in your claim and billing processes. By taking a proactive approach to Denial Management, cash flows are increased, and overall cost to collect is reduced.
Let’s talk about how we can help to reduce your initial denial rate altogether and help to make appeals more efficient for your organization. Contact ReMedics today to get started.
